BiothreatsAntimicrobial resistance: A neglected biodefense vulnerability
We typically think that biodefense is about defending against bioterrorism or the next pandemic – or, in extreme cases, about some laboratory accident. Biodefense is mostly about all these things, but also about much more. Antimicrobial resistance is not a headline-grabbing topic and it certainly is not getting its own apocalyptic outbreak movie anytime soon, but the microbial threat has been growing since antibiotics were first discovered.
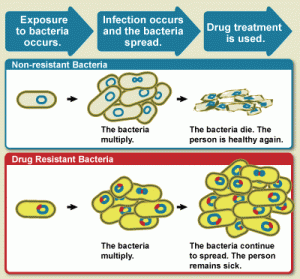
Path to antibacterial reasistance // Source: commons.wikipedia.org
We typically think that biodefense is about defending against bioterrorism or the next pandemic – or, in extreme cases, about some laboratory accident.
Pandora Report notes that biodefense is mostly about all these things, but also about much more.
Antimicrobial resistance is not a headline-grabbing topic and it certainly is not getting its own apocalyptic outbreak movie anytime soon, but the microbial threat has been growing since antibiotics were first discovered.
Pew Charitable Trusts has been working hard to combat anti-microbial resistance (AMR), and recently discussed the role it has in U.S. biodefense efforts.
Rick Bright, director of the Biomedical Advanced Research and Development Authority (BARDA)—part of the Department of Health and Human Services’ Office of the Assistant Secretary for Preparedness and Response, is among those leading the U.S. biodefense strategy’s implementation. In a recent interview with Pew (“Fight against superbugs crucial to America’s biodefense: How the U.S. is countering the national security threat posed by antibiotic-resistant bacteria,” Pew Trust, 1 February 2019), he discussed the threat posed by antibiotic-resistant bacteria and the work underway to mitigate the risks.
He said:
Antibiotic-resistant bacteria are not only a threat to public health in the United States, but also to national security. The federal government has recognized that antibiotic-resistant pathogens complicate soldiers’ wounds, exacerbate casualties associated with both natural and manmade emergencies, and can be weaponized by our nation’s enemies. Consequently, the first U.S. National Biodefense Strategy, released last year, highlights the need to reduce the emergence and spread of such superbugs both domestically and internationally, and accelerate the development of new drugs, diagnostic tests, and vaccines. Rick Bright, director of the Biomedical Advanced Research and Development Authority(BARDA)—part of the Department of Health and Human Services’ Office of the Assistant Secretary for Preparedness and Response—is among those leading the strategy’s implementation.
He added:
We need new and better methods of disease detection, including tests at home, in urgent care centers and in the doctor’s office that can tell immediately whether you have a viral or bacterial infection, and which antibiotics to use or to avoid. We’re working on that with private partners. We also need new and innovative classes of antibiotics that combat resistant bacterial infections and that are less vulnerable to emergence of resistance; we’re working on that with private partners, too. We must invest in alternative approaches to treating bacterial infections with drugs and include more vaccines in our arsenal. Finally, we must also identify common ways our bodies respond to disease. This will enable us to target treatments to the individual so that they can manage severe inflammation and other biological responses that can sometimes cause more harm than the invading organism.
Technology and science aside, the U.S. and global community still needs to address the market entry lag and challenge of sustaining the fragile antibiotic industry. Perhaps the time has come to consider additional business models for development, production and distribution of antibiotics.
